Dear Retroflexions,
Over two years ago, I had a colon resection for the removal of a cancerous tumor (stage 2A). Ever since, I have had on and off bleeding in my stool. My surgeon has done two sigmoidoscopies and my gastro doctor has done two colonoscopies. The findings as of November 2015 are granulation tissue at the resection site (sigmoid). The bleeding comes and goes… maybe 2 weeks to a month…no blood…then it starts again. Its been back since July 1st.
The biopsies have all shown granulation tissue (benign).
Have you every had a patient like me? My doctors say I worry to much.
-Mr. M
(update, 5 days later)
Here is an update. I had another sigmoidoscopy yesterday.
The granulation tissue is gone and has been replaced by “vascular proliferation at the anastamosis.”
I have attached a picture.
Please do a blog about this soon if you can.
Thank You,
-Mr. M
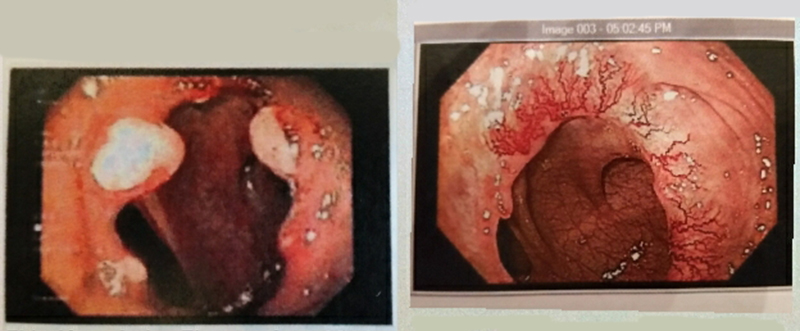
Left: Appearance of anastomosis several months after surgery with signs of active healing/granulation tissue. Right: Two years after surgery there is a proliferation of blood vessels at anastomosis.
An anastomosis is a surgical connection of two hollow organs: In this patient’s case there was a tumor in the sigmoid colon that was removed, and the surgeon attached the two cut ends of the remaining colon together to make a working colon again. Like any wound, the anastomosis undergoes a healing process after surgery. Part of this process is the growth of new blood vessels into the anastomosis, and it seems like in the above case there is an overabundance of abnormal-appearing blood vessels growing all over the anastomosis. These blood vessels appear superficial and friable, and are prone to spontaneous bleeding. I would say they could be called telangiectasias, or angioectasias, or this could be called overabundant neovascularization of the anastomosis, or as the author of the report stated “vascular proliferation at the anastomosis.”
A few questions come to my mind when seeing a case like this: 1)Why does this happen; 2)Is this condition harmful; 3)How could we treat this condition to reduce the frequent bleeding; and finally, 4)What is the natural history of this problem if left untreated?
To preface the rest of this article, I don’t necessarily have the answers to questions 1-4 above! However, I have seen several cases like this, so here are some of my (probably oversimplified) thoughts on the topic: Whenever there is an abnormal proliferation of vascular tissue in the GI tract, we gastroenterologists should ask ourselves “what forces created this lesion?” For example, when we see esophageal varices, we think about portal hypertension, when we see colonic angiodysplasia we think of a multitude of risk factors. When I see angioectasias related to an anastomosis, I think of ischemia as the inciting factor. That is, there is limited blood flow to the tissue at the site of the anastomosis, as the natural blood supply has been disrupted by surgery, and there are now staples or sutures squeezing the tissue together. However, the anastomosis needs oxygen (in the form of blood flow) to heal, so it sends signals out locally to tell the body to hurry up and grow some new blood vessels to supply the healing tissue. These signals come in the form of a substance called vascular endothelial growth factor (VEGF).
VEGF makes the blood vessels grow alright, but sometimes the way they grow ain’t pretty. The new vessels can grow erratically and in excess, and we have what you see in the pictures above. Is it harmful? Probably not, except for the occasional (usually minor) bleeding episodes. In patients that bleed frequently from these anastomotic vascular lesions, I have treated the vessels with cautery or clips to stop or prevent the bleeding. It seems to work quite well, but I am always thinking that since I did nothing to treat the underlying problem of tissue-level ischemia that new funny-looking blood vessels will probably just grow back again at some point..and they often do.
What about just leaving this alone? Maybe the healing process is ongoing and in another year or two most of these vessels will self-destruct as the anastomosis fully matures. Or maybe deeper, more effective vessels will grow in, and therefore after we ablate these superficial angioectasias there will no longer be ongoing ischemia at the anastomosis, and new vessels will not be needed to repopulate the area? Perhaps this is all just wishful thinking? In extreme cases of anastomotic bleeding, sometimes the surgery has to be revised: The old anastomosis is resected and a new one is made, and hopefully the same problem does not happen again.
References:
Bosmans JW, Jongen AC, Bouvy ND, et al. Colorectal anastomotic healing: why the biological processes that lead to anastomotic leakage should be revealed prior to conducting intervention studies. BMC Gastroenterol 2015;15:180.
Scappaticci FA, Fehrenbacher L, Cartwright T, et al. Surgical wound healing complications in metastatic colorectal cancer patients treated with bevacizumab. J. Surg Oncol 2005;91:173-180.
Tanaka IM, Sugio IT, Tanaka ST, et al. Local VEGF administration enhances healing of colonic anastomoses in a rabbit model. Eur Surg Res 2009;42:249-57.