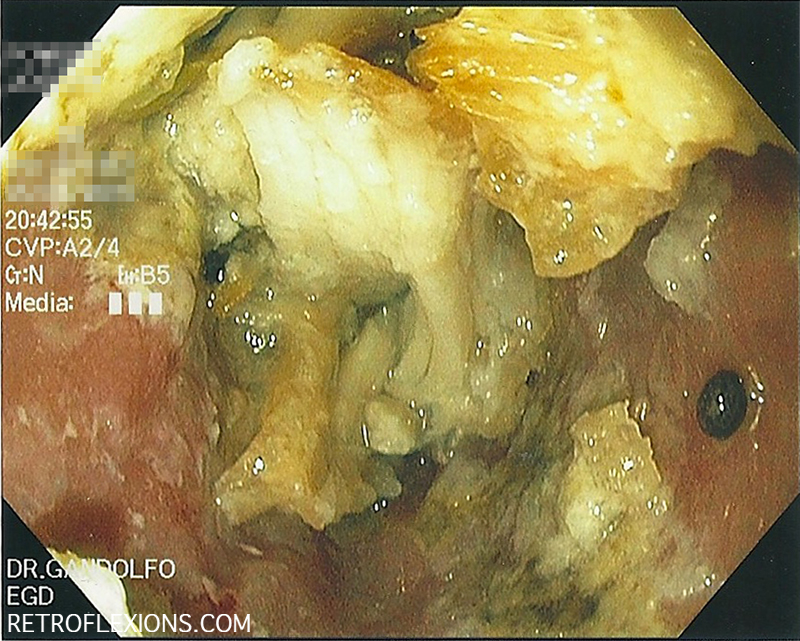
Food impaction in the esophagus is one of the emergency conditions that only gastroenterologists and emergency room doctors know about. The overall concept is simple: Soon-to-be patient eats a large quantity of food (most commonly meat), which gets stuck in the esophagus somewhere and then causes a blockage and prevents further swallowing. Patient experiences chest pain, foreign body sensation, drooling, and generalized sense of discomfort and proceeds to come to the emergency room. ER doctor calls GI doctor and (usually) endoscopy is performed. The blockage is relieved and the patient goes home.
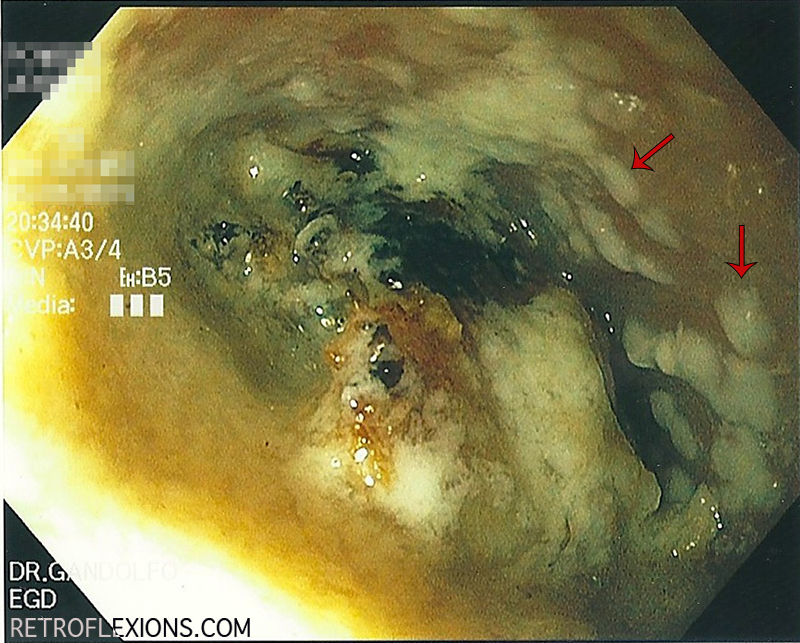
The appearance of a food impaction that has been present for more than 48 hours. The white-colored creamy plaques (red arrows) are probably colonies of yeast or bacteria already growing on the esophageal wall.
Most food impactions happen in people who already have some type of esophageal pathology in the first place. Esophageal rings, strictures, tumors, inflammation, and a condition called eosinophilic esophagitis are the common conditions that can lead to food impaction. Meat (whole pieces of steak, chicken, pork, lobster, etc.) is the most common food to cause an impaction since it is solid and does not break apart into smaller pieces over time as a piece of bread would do.
In my anecdotal experience, most food impaction calls happen around 10-11 PM, or first thing in the morning. Dinner is usually the meal that causes the food impaction, and most people try to wait it out for 3-5 hours before eventually getting frightened and coming to the ER late at night. Others try to “sleep it off” only to find that the problem is still there in the morning, so they come in at 7 AM. So food impactions are a somewhat common GI emergency when on call. Within reason, most food impaction cases should be scoped as soon as possible. However, all food impaction cases should be scoped within 24 hours of the event, since after 24 hours the risk of complications such as esophageal perforation rises. But what about the patient who presents to the hospital after the impaction has already been present for more than 24 hours?
The following images illustrate a case of food impaction in a 58-year-old man that presented to the hospital after 48 hours of not being able to swallow after eating pork. The patient was spitting saliva into a cup (which in my experience is 100% predictive of finding a food impaction on endoscopy) and was complaining of chest pain.
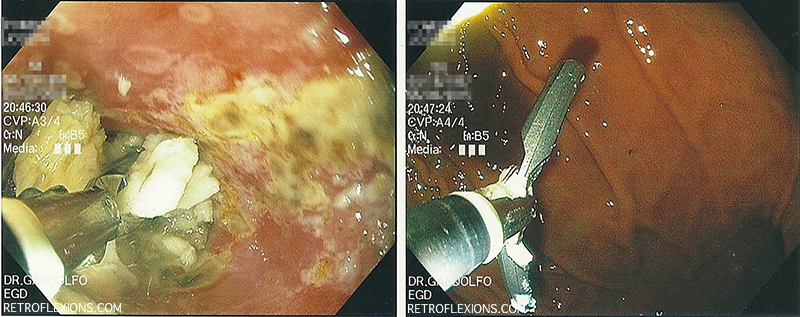
Alligator forceps are used to remove the meat from the esophagus: (L) using the forceps in the esophagus; (R) showing the large size of the open forceps in the stomach.
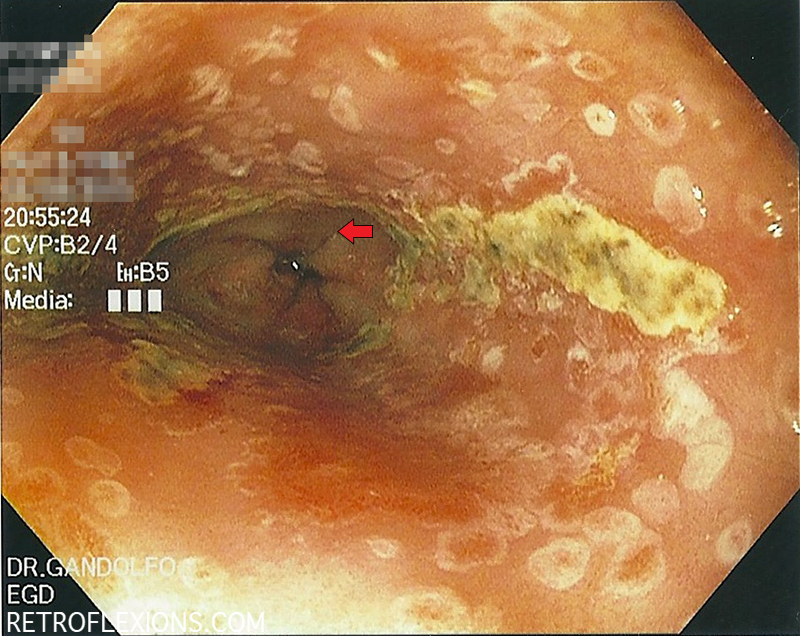
The esophagus after the food impaction was removed. Note the ulceration and exudate from prolonged stasis of food and bacteria in the distal esophagus. The top of the gastric folds (red arrow) define the gastroesophageal junction.
How does one avoid a food impaction? Since most cases happen in patients with an abnormal esophagus, promptly addressing any dysphagia (trouble swallowing) and not letting it get to this point is critical. Big problems usually start as small problems and get worse over time. Lastly, it may be common sense, and mothers around the world have been saying it forever, but taking smaller bites, and chewing your food well may also help prevent these type of incidents.
If you enjoyed this article, sign up for our free newsletter and never miss a post!
Written informed consent was obtained from the patient prior to publication of this case report.